Understanding
Charcot Foot
Greg Mack, DPM, FACFAS
Podiatric Medicine
Foot and Ankle Clinic
Menomonie
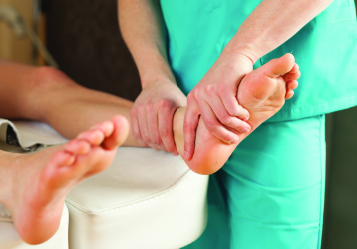 What Is Charcot Foot?
What Is Charcot Foot?
We as practitioners are entering a whole new realm of medicine. As research is finding cures and treatment plans for a multitude of diseases we are at risk of becoming complacent with our successes. We often ask ourselves what is the new and problematic condition that will be sent to us in the future.
With the current obesity epidemic, our population is at risk of developing diabetes at an alarming rate. With the diagnosis of a diabetic condition we need to educate our patients regarding the complications of diabetes. One complication that can arise is the development of neuropathic changes of the foot and ultimately the serious deformity of Charcot arthropathy. Charcot foot is a condition that causes weakening of the bones in the foot and can occur in people who have significant nerve damage (neuropathy). The bones are weakened enough to fracture, and with continued walking, the foot eventually changes shape. As the disorder progresses, the joints collapse and the foot takes on an abnormal shape, such as a rocker-bottom appearance.
Charcot foot is a serious condition that can lead to severe deformity, disability and even amputation. Because of its seriousness, it is important that patients living with diabetes—a disease often associated with neuropathy (weakness, numbness, and pain in the foot)—take preventive measures and seek immediate care if signs or symptoms of Charcot appear. We as foot specialists need to help you understand what to look out for.
Causes
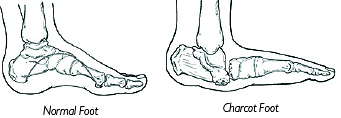 Charcot foot develops as a result of neuropathy, which decreases sensation and the ability to feel temperature, pain or trauma. Because of diminished sensation, the patient may continue to walk—making the injury worse. People with neuropathy (especially those who have had it for a long time) are at risk for developing Charcot foot. In addition, neuropathic patients with a tight Achilles tendon have been shown to have a tendency to develop Charcot foot.
Charcot foot develops as a result of neuropathy, which decreases sensation and the ability to feel temperature, pain or trauma. Because of diminished sensation, the patient may continue to walk—making the injury worse. People with neuropathy (especially those who have had it for a long time) are at risk for developing Charcot foot. In addition, neuropathic patients with a tight Achilles tendon have been shown to have a tendency to develop Charcot foot.
Diagnosis—Prevention is the Key
Early diagnosis of Charcot foot is extremely important for successful treatment. To arrive at a diagnosis, the surgeon will examine the foot and ankle and ask about events that may have occurred prior to the symptoms. X-rays and other imaging studies and tests may be ordered. Once treatment begins, x-rays are taken periodically to aid in evaluating the status of the condition.
Nonsurgical Treatment
It is extremely important to follow the surgeon’s treatment plan
for Charcot foot. Failure to do so can lead to the loss of a toe, foot, leg, or life.
Nonsurgical treatment for Charcot foot consists of:
- Immobilization
Because the foot and ankle are so fragile during the early stage of Charcot, they must be protected so the weakened bones can repair themselves. Complete nonweightbearing is necessary to keep the foot from further collapsing. The patient will not be able to walk on the affected foot until the surgeon determines it is safe to do so. During this period, the patient may be fitted with a cast, removable boot, or brace and may be required to use crutches or a wheelchair. It may take the bones several months
to heal, although it can take considerably longer in some patients.
- Custom shoes and bracing
Shoes with special inserts may be needed after the bones have healed to enable the patient to return to daily activities—as well as help prevent recurrence of Charcot foot, development of ulcers, and possible amputation. In cases with significant deformity, bracing is also required.
- Activity modification
A modification in activity level may be needed to avoid repetitive trauma to both feet. A patient with Charcot in one foot is more likely to develop it in the other foot, so measures must be taken to protect both feet.
When Is Surgery Needed?
In some cases, the Charcot deformity may become severe enough that surgery is necessary. The foot and ankle surgeon will determine the proper timing as well as the appropriate procedure for the individual case.
Preventive Care
The patient can play a vital role in preventing Charcot foot and its complications by following these measures:
- Keeping blood sugar levels under control can help reduce the progression of nerve damage in the feet.
- Get regular checkups from a foot and ankle surgeon.
- Check both feet every day—and see a surgeon immediately if you notice signs of Charcot foot.
- Be careful to avoid injury, such as bumping the foot or overdoing an exercise program.
- Follow the surgeon’s instructions for long-term treatment to prevent recurrences, ulcers, and amputation.
It has been my experience over my 27 years of practice that we can totally avoid the risk of the ultimate complication, amputation, with early intervention. Recognizing that a patient has risk factors is key. I feel that everyone who is at risk of Charcot arthropathy must comply with aggressive motion controlling inserts and I have had excellent success in avoiding collapse of the bone with devices called UCBL gait plates. These only work if we recognize the condition early in the process. I prescribe and fit mechanical inserts in diabetics that show beginning signs of neuropathy as well. The most devastating thing that I have to say in my practice is “we cannot save your leg”. Fortunately in my practice this is something that I rarely have to tell patients as we strive to be proactive.
It would be nice if we can abolish the diabetic condition and the risk of developing Charcot arthropathy. We as practitioners must inform our patient population that obesity often leads to diabetes and the conditions that result can cause disabilities and shorten one’s life span significantly and the majority of these symptoms can be prevented by controlling your weight.
Dr. Mack – Foot and Ankle Clinic
For information or to schedule an appointment:
715-235-4274 | 800-359-4421 | footankle-clinic.com
Dr. Mack sees patients in Menomonie, Cumberland, Eau Claire, Rice Lake,
Shell Lake and Hayward.